
Greppi Award 2018
The period preceding a migraine attack is often associated with abnormal sensory processing in the brain1, and hyper-responsivity is the most common electrophysiological characteristic observed in patients with episodic migraine during the interictal phase.2 Abnormal cerebral metabolism has also been implicated in migraine, and the metabolic strain hypothesis proposes that reduced energy supplies in the cortex between attacks may lead to the brain being unable to cope with this hyperactive neuronal activity.2
The Enrico Greppi Award, endorsed by the European Headache Federation (EHF), is presented every year to an unpublished original paper that examines epidemiological, genetic, pathophysiological or therapeutic aspects of headache (Figure 1).3
The Award is supported through an educational grant by TEVA Neuroscience. The article selected for this year’s award, which was presented to Dr Marco Lisicki at the EHF 2018 meeting in Florence, examined whether interictal glucose metabolism in the visual cortex is proportional to visually induced neuronal activation among 20 patients with episodic migraine without aura and 20 healthy volunteers.2 In the study, 18-fluorodeoxyglucose positron emission tomography (18-F-FDG PET) was used to measure resting cerebral glucose uptake, and visual evoked potentials were used to evaluate the responsiveness of the visual cortex.2
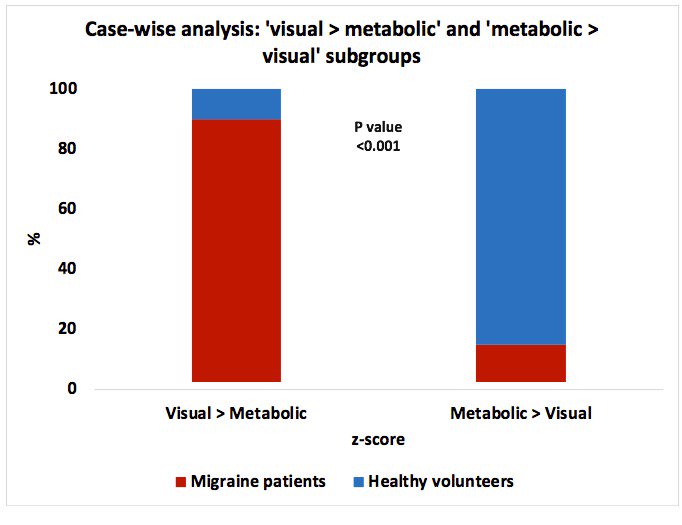
The study showed that visual cortex responsiveness was significantly greater in patients with migraine, compared with healthy controls – an observation that concurs with previous studies.2 Most interestingly, the ratio of stimulation-induced neuronal activation to resting glucose uptake was significantly higher in patients with migraine compared with healthy individuals.2 Furthermore, the researchers were able to identify a specific region of the visual cortex in which this difference in ratio was greatest. Within this area, visual neuronal activation exceeding glucose uptake was observed in 90% of patients with migraine and in only 15% of healthy controls (Figure 2). 2
The findings by Dr Lisicki and colleagues provide evidence supporting the idea that metabolic strain contributes to the generation of the attack in its initial phase and suggest that the physiological sensory–metabolic equilibrium is abnormal between migraine attacks.2 Unmet neuronal metabolic demands could eventually result in the release of molecules that activate the brain’s major alarm system, the trigeminovascular system, leading to the initiation of a migraine attack, with the aim of re-establishing cortical homeostasis.2
In summary, the results of this study indicate that in many patients with migraine, there is an area of the visual cortex in which there is an increased ratio of neuronal activation to resting glucose uptake. This is an exciting observation supporting the idea that an activity-induced disruption or dysregulation of cerebral metabolic homeostasis could be a key feature of migraine pathophysiology.2
Goadsby PJ, Holland PR, Martins-Oliveira M, Hoffmann J, Schankin C, Akerman S. Pathophysiology of Migraine: A Disorder of Sensory Processing. Physiol Rev 2017; 97(2): 553-622.
Lisicki M, D'Ostilio K, Coppola G, Scholtes F, Maertens de Noordhout A, Parisi V, Schoenen J, Magis D. Evidence of an increased neuronal activation-to-resting glucose uptake ratio in the visual cortex of migraine patients: a study comparing (18)FDG-PET and visual evoked potentials. J Headache Pain 2018; 19(1): 49.
SISC. Enrico Greppi Award. Available at: https://www.sisc.it/eng/enrico-greppi-award_30.html



